A dive into Generalized Anxiety Disorder (GAD) and Major Depressive Disorder (MDD) during and after the COVID-19 Pandemic.
“We need a refuge even though we may never go there. I may never in my life get to Alaska, for example, but I am grateful that it’s there. We need the possibility of escape as surely as we need hope…” – Edward Abbey, Desert Solitaire.
To avoid “burying the lede” as the journalists say, people afflicted with – or those at risk of – MDD and GAD faired quite poorly during the pandemic. People afflicted with MDD and GAD are also a great lens with which to analyze the problems that COVID-19 brought to light.
I am discussing MDD and GAD together because they often go hand-in-hand and in some situations can be treated in similar ways. When looking into GAD and MDD it is important to recognize that they are diagnosed disorders. This also means that they have very specific criteria that must be met. In many of the studies that I will be referring to, there are self-reporting questionnaires used to see if people meet the different criteria for GAD or MDD.
Without knowledge of the criteria for GAD and MDD it is hard to use them as a viewfinder for other mental health issues. Below is a list of criteria for each, their shared characteristics are italicized (Zbozinek et al.):
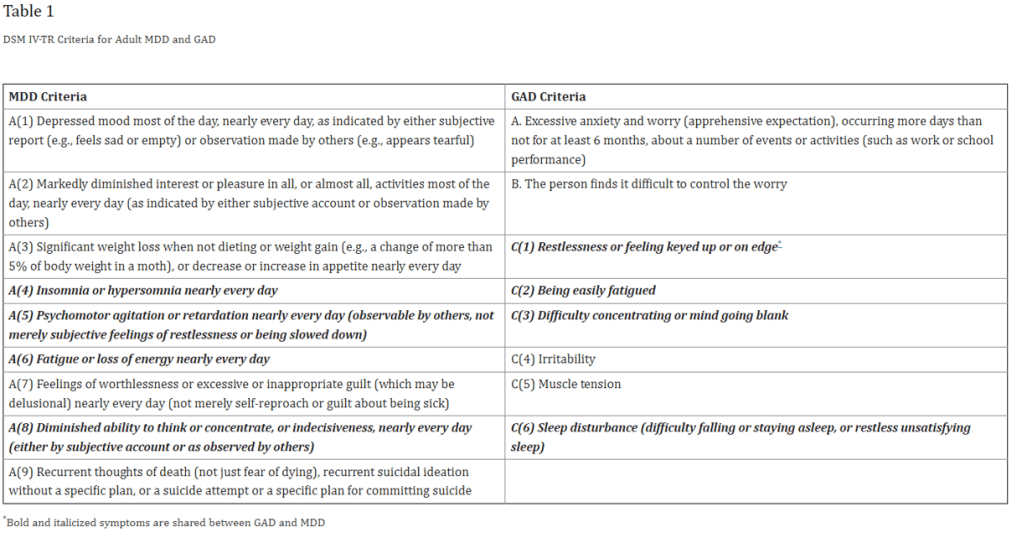
While MDD and GAD cannot be further simplified without losing something, and at the risk of showing my hubris, I think it can be likened to the quote at the beginning of this post. Meaning that, MDD is like an overall loss of hope, while GAD is like an overall loss of the possibility of escape.
When thought of in these terms of hope and escape, It makes perfect sense that the Coronavirus Pandemic caused problems for those afflicted – or those to be afflicted – with MDD or GAD symptoms. The COVID-19 Pandemic caused many of us to lose hope after it seemed to get a weekly extension, while simultaneously worsening for over two years. The possibility of escape also seemed rather unattainable, as the pandemic raged across the globe, and its effects were felt everywhere. These effects were felt in both the real and virtual worlds. A person couldn’t so much as go onto their phone without seeing a barrage of doomsday information on COVID-19.
*****
Here, I am going to dive into the weeds of the studies about the Coronavirus Pandemic and MDD/GAD, f you are interested in skipping this part, you can jump to the “*****” below.
The effects of the COVID-19 Pandemic on people who had, or were predisposed to having, MDD or GAD can be analyzed in two distinct ways. The first is looking at the effects that COVID-19 had on people who caught it, while the second is analyzing the effect that the overall pandemic had on people.
First, Monistrol-Mula et al. wrote a paper titled, The impact of COVID‑related perceived stress and social support on generalized anxiety and major depressive disorders: moderating effects of pre‑pandemic mental disorders. In this paper, the authors break down the different potential causes for increases in GAD and MDD. I will avoid boring you with all of the details, but they did a great job of mitigating things that would call the legitimacy of the study into question. As is the case in all my posts, you can view the methods for yourself by following the citation at the bottom of this post.
Monistrol-Mula et al. broke up the data into many different categories and found that people with a positive infection status were more likely to screen positive for MDD or GAD. The positivity rate for GAD without COVID-19 was 10.83%, while the positivity rate for GAD with COVID-19 was 13.62%. Similarly, the positivity rate for MDD without COVID-19 was 11.14%, while the positivity rate with COVID-19 was 15.41%. Interestingly, for the combination of MDD and GAD the percentages were 6.72% (without COVID-19) and 3.34% (with COVID-19). I believe that this comes from an exceedingly low sample size of n=242 with both GAD and MDD, as opposed to n=395 and n=407 respectively.
As a quick little aside, while this matches with intuition for an illness making one’s anxiety or depression worse, I would be quick to point out that these values are not large enough to be considered statistically significant. As such, we should definitely have more retrospective studies in this era following the Coronavirus Pandemic.
The public anxiety and lack of a cohesive social network has impacted all people regardless of whether they had COVID-19 or not. For people without a history of mental illness, GAD and MDD jumped approximately 5.59% and 5.87% respectively (Monistrol-Mula et al.). This is nuts, especially if you extrapolate it to the rest of the population.
A study conducted by Aboul-ata et al in Egypt further analyzed the correlation between the effects of COVID-19 and MDD/GAD. This study used the Patient Health Questionnaire (PHQ-9) to assess MDD, and the Generalized Anxiety Disorder-7 (GAD-7) to assess GAD. The study had 7015 participants and resulted in statistically significant results for four of five expected factors. The four factors were Anxiousness, Social Support, Avoiding/Cleaning, and Medical Concern. The study did not find correlation for Deppresivity. This means that the data from the first study, which was conducted in Spain, is supported from a different study – with slightly different methods – in Egypt.
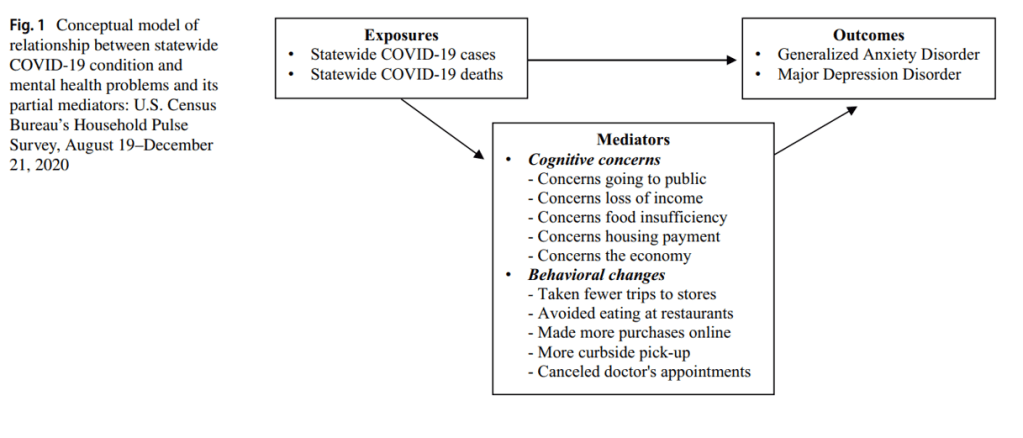
After looking at Spain and Egypt, let us look at a study that was conducted in the good old US of A; COVID‑19 pandemic and mental health problems of adults in United States: mediating roles of cognitive concerns and behavioral changes. In a previous study conducted in China, it was established that having a strong social network correlated with lower risk of GAD and MDD (Z. Ma et al.). This study used this information and conducted a large statistical analysis of all 50 states. The study used the COVID-19 infection numbers, as well as the Household Pulse Survey (HPS). The HPS was taken in three 3 to 4 month phases that were all recorded in 2020. The results of this study further corroborated the results of the studies in Spain, China, and Egypt, and can be visualized in the excellent diagram that was “Figure 1” in the paper (JungHo Park et al.):
*****
So, what does all this mean for us?
The Coronavirus Pandemic resulted in increased anxiety and depression for individual people. The results were worse if a person had any history of mental illness, or actually contracted COVID-19. Similarly, if a person had a poor social network they were at further risk.
I also want to hammer home that these studies were looking at GAD and MDD, meaning that they were not looking at people who just had a rough time during the COVID-19 pandemic. For every person with MDD or GAD there were many more who were anxious and depressed to a less clinical level, and that cannot be discounted.
When we see these increases in mental illness it’s time to look at the system that’s causing it and not just the people getting sick. Just like in traditional medicine, it is better to be proactive than reactive.
Again, for people with no history of mental illness, rates of GAD and MDD jumped approximately 5.59% and 5.87% respectively. This doesn’t happen overnight in a stable society. This jump of almost 6% was for a diagnosable disease, imagine the people who didn’t have a diagnosable jump in depression or anxiety but a drastic one, nevertheless.
This research really goes to show that we are not living in a society that is ready to cope with largescale challenges (pandemics, climate disasters, technological advances, etc., etc.). Many of the ill-effects of the pandemic, were a result of panic portrayed by the media as well as our social networks, which are much further reaching than they once were – I discussed this in The Invisible Pandemic (Part I).
It would not be catastrophizing to say that the problems that caused a drastic increase in MDD and GAD during the COVID-19 area are not going anywhere, even as the Coronavirus Pandemic comes to an end.
MDD and GAD provide us a great quantifiable lens with which to analyze the truly awful effects that COVID-19 brought to light. Going forward, we need to take a long, deep look at our support systems, our news sources, and our social media.
In my next post, I am going to continue with some of the steps that we can take to reduce the effects that were felt during the Pandemic. I see very little value in bringing problems to light without analyzing their potential solutions. As such, I will be looking at everything from startups doing great work, to charities making a difference, too little day-to-day steps that we all can take.
In the meantime, however, I would posit to you that our oh-so-precious news networks and social media apps are taking away the refuge that we once enjoyed in our close support networks. Without this refuge, I leave you with the words of Edward Abbey:
“We need a refuge even though we may never go there. I may never in my life get to Alaska, for example, but I am grateful that it’s there. We need the possibility of escape as surely as we need hope…” – Edward Abbey, Desert Solitaire.
Citations
Aboul-ata, & Qonsua, F. T. (2021). The 5-factor model of psychological response to COVID-19: its correlation with anxiety and depression. Current Psychology (New Brunswick, N.J.), 41(1), 516–528. https://doi.org/10.1007/s12144-021-01701-y
Li, Cao, H., Leung, D. Y. P., & Mak, Y. W. (2020). The Psychological Impacts of a COVID-19 Outbreak on College Students in China: A Longitudinal Study. International Journal of Environmental Research and Public Health, 17(11), 3933. https://doi.org/10.3390/ijerph17113933
Ma, Zhao, J., Li, Y., Chen, D., Wang, T., Zhang, Z., Chen, Z., Yu, Q., Jiang, J., Fan, F., & Liu, X. (2020). Mental health problems and correlates among 746 217 college students during the coronavirus disease 2019 outbreak in China. Epidemiology and Psychiatric Sciences, 29, e181–e181. https://doi.org/10.1017/S2045796020000931
Monistrol-Mula, Félez-Nobrega, M., Domènech-Abella, J., Mortier, P., Cristóbal-Narváez, P., Vilagut Saiz, Gemma, 1975, Olaya, B., Ferrer, M., Gabarrell-Pascuet, A., Alonso Caballero, J., & Haro Abad, J. M. (2022). The impact of COVID-related perceived stress and social support on generalized anxiety and major depressive disorders: moderating effects of pre-pandemic mental disorders. https://doi.org/10.1186/s12991-022-00385-3
Park, Choi, J., & Kim, B. (2022). COVID-19 pandemic and mental health problems of adults in United States: mediating roles of cognitive concerns and behavioral changes. Social Psychiatry and Psychiatric Epidemiology, 57(8), 1557–1570. https://doi.org/10.1007/s00127-022-02265-3
Wang, Pan, R., Wan, X., Tan, Y., Xu, L., Ho, C. S., & Ho, R. C. (2020). Immediate Psychological Responses and Associated Factors during the Initial Stage of the 2019 Coronavirus Disease (COVID-19) Epidemic among the General Population in China. International Journal of Environmental Research and Public Health, 17(5), 1729. https://doi.org/10.3390/ijerph17051729
Zbozinek, Rose, R. D., Wolitzky-Taylor, K. B., Sherbourne, C., Sullivan, G., Stein, M. B., Roy-Byrne, P. P., & Craske, M. G. (2012). DIAGNOSTIC OVERLAP OF GENERALIZED ANXIETY DISORDER AND MAJOR DEPRESSIVE DISORDER IN A PRIMARY CARE SAMPLE. Depression and Anxiety, 29(12), 1065–1071. https://doi.org/10.1002/da.22026

One thought on “The Invisible Pandemic (Part II)”